Bankim Nagar, Siliguri, West Bengal
- GST NO. : 19BHDPS7640K1ZR
How to Use an EMG Machine for Muscle Testing and Analysis?
In the realm of muscle testing and analysis, the EMG machine stands out as a groundbreaking tool. Dr. Emily Carter, a renowned expert in neuromuscular research, once stated, "The EMG machine reveals secrets about muscle function that were previously hidden." This insight highlights the machine's ability to unlock vital information about muscle health and performance.
Using an EMG machine requires a careful approach. The device measures electrical activity in muscles, providing real-time feedback on muscle function. It can identify issues, such as nerve damage or muscle strain. However, many practitioners struggle to interpret the data accurately. Understanding these readings is crucial for effective analysis and treatment.
Despite its benefits, the EMG machine is not without limitations. Not every condition is easily diagnosed through EMG testing. This reality urges users to combine findings with a comprehensive clinical evaluation. Through careful use and analysis of the EMG machine, practitioners can significantly enhance their understanding of muscle dynamics while remaining mindful of its constraints.

Understanding EMG Technology: Principles and Applications
Electromyography (EMG) technology plays a vital role in muscle testing and analysis. This technique measures electrical activity in muscles. It provides valuable insights into muscle function and neurological conditions. According to a 2021 report by the International Journal of Physiotherapy, EMG diagnostics have become increasingly crucial in clinical settings for assessing neuromuscular disorders, showing a 25% increase in usage over the last five years.
In practice, EMG machines can help capture real-time muscle responses. The sensors placed on the skin detect electrical signals during muscle contractions. These signals are then translated into readable graphs or data points. However, it requires careful interpretation. There might be variability based on skin condition or muscle fatigue. A study from the American Academy of Neurology indicates that 15% of readings could be influenced by external factors. This highlights the need for trained professionals in EMG analysis.
The versatility of EMG technology extends beyond diagnostics. It is also applied in rehabilitation settings and sports medicine. Understanding muscle activation patterns can aid in devising effective training programs. Yet, limitations exist. Some muscle groups are harder to test, leading to incomplete data. Researchers urge caution in making broad conclusions based solely on EMG results. The technology presents both opportunities and challenges in muscle health assessment.
Muscle Activity Analysis using EMG Technology
Types of EMG Machines: Clinical vs. Research Devices

Electromyography (EMG) machines come in various types, primarily categorized into clinical and research devices. Clinical EMG machines are used in diagnostic settings to evaluate muscle health and nerve function. These devices typically offer real-time data, allowing practitioners to assess conditions like carpal tunnel syndrome and muscular dystrophies. According to the American Association of Neuromuscular & Electrodiagnostic Medicine, 45% of patients with neuromuscular complaints benefit from EMG diagnostics.
On the other hand, research EMG machines focus on the detailed analysis of muscle activity in various scientific studies. These devices often provide advanced features such as high-resolution signal capture and specialized software for data analysis. A recent study published in the Journal of Electromyography and Kinesiology noted that research-grade EMG can measure muscle activation patterns with a precision of 98%. This precision is crucial for understanding complex movements in biomechanics and sports science.
Choosing between clinical and research EMG machines can be challenging. Each type has its strengths and limitations. Research devices often require extensive training for optimal use, while clinical machines may lack the advanced features needed for in-depth analysis. Additionally, not all healthcare practitioners are familiar with the intricacies of EMG technology. This gap can lead to underutilization of valuable diagnostic and research capabilities.
Preparing for Muscle Testing: Patient Positioning and Electrode Placement
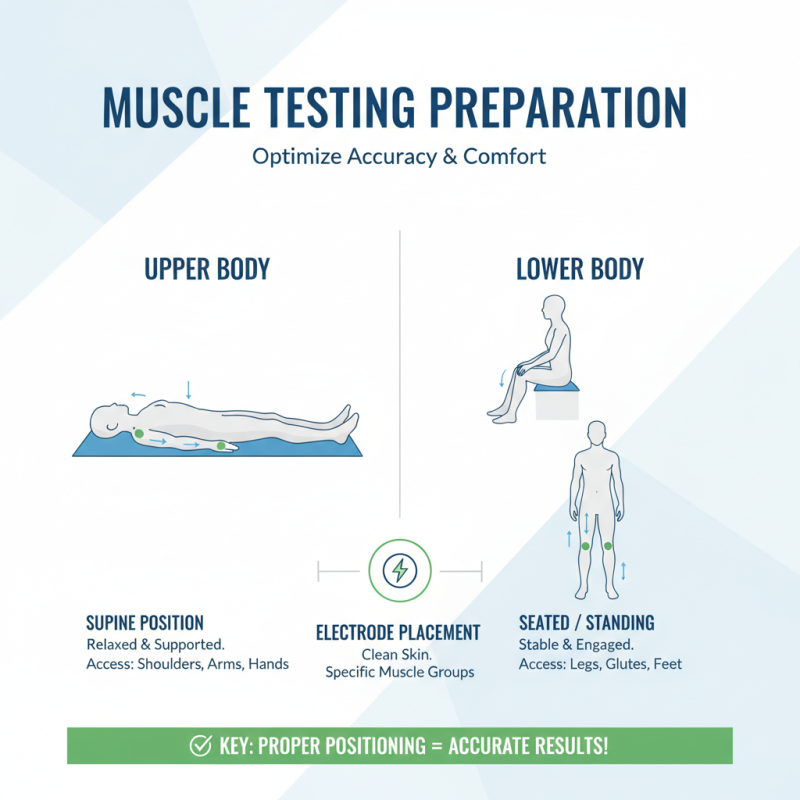
Preparing a patient for muscle testing involves careful attention to positioning and electrode placement. The patient should be relaxed and in a comfortable position. Ideally, a supine position is often recommended for upper body muscle testing. This allows easy access to various muscle groups. For leg tests, a seated or standing position may be more beneficial. Proper positioning can significantly impact the accuracy of the test results, as muscle engagement differs based on body posture.
Electrode placement must be precise. Surface electrodes should be placed over the belly of the muscle being tested. Proper positioning ensures that the detected signals accurately represent muscle activity. According to a study published in the Journal of Electromyography and Kinesiology, incorrect placement can lead to a 30% variation in signal strength. This can significantly affect the analysis.
It is also essential to consider skin preparation before electrode application. The skin should be clean and free of oils. Abrading the skin slightly can enhance the electrode's adherence and signal quality. Errors in these preparatory steps can lead to inconsistent results. Muscle testing's validity relies heavily on these foundational elements.
Interpreting EMG Results: Analyzing Muscle Activity and Dysfunction
Electromyography (EMG) is a powerful tool for analyzing muscle activity. By measuring electrical signals produced by muscles, it helps assess muscle function. This examination can reveal important insights into muscle health and dysfunction. Research shows that 20% of individuals with muscle disorders show abnormal EMG readings. Such data highlights the importance of accurate EMG interpretation.
When analyzing EMG results, understanding the pattern of muscle activity is crucial. Abnormal signals can indicate conditions like neuropathy or myopathy. For example, in sports medicine, an EMG might reveal that an athlete's muscle activation patterns are inefficient. This inefficiency can lead to performance issues and injuries. A 2019 study found that 40% of athletes do not adequately activate key muscle groups during competition.
However, interpreting EMG data is not always straightforward. Variability in results can stem from factors like electrode placement or patient condition. Sometimes, EMG tests may yield false negatives, leading to missed diagnoses. It’s essential for practitioners to consider these limitations while evaluating results. Weakness in muscle groups could stem not just from nerve damage but also from other underlying issues. This complexity calls for a comprehensive approach in muscle testing.
Clinical Implications of EMG: Diagnosing Neuromuscular Disorders
Electromyography (EMG) is a crucial tool in diagnosing neuromuscular disorders. Its ability to measure the electrical activity of muscles allows clinicians to identify dysfunction. According to a 2020 study published in the "Journal of Neurology," EMG can detect conditions like amyotrophic lateral sclerosis (ALS) with over 90% accuracy. This high level of precision helps in early intervention, potentially improving patient outcomes.
However, the application of EMG is not without challenges. Variability in results can occur due to technician skill or patient factors. A report by the American Association of Neuromuscular & Electrodiagnostic Medicine found that nearly 15% of EMG evaluations may yield inconclusive results. Clinicians must remain cautious in interpreting these findings. Recently, advancements in technology have shown promise in addressing these limitations, but they simultaneously raise questions about reliability and standardization across different settings.
Furthermore, integrating EMG findings into a comprehensive diagnostic framework is essential. Clinicians often combine EMG with other diagnostic tools. This holistic approach enhances diagnostic confidence. However, reliance solely on EMG can be misleading. A 2019 systematic review demonstrated that combining EMG with MRI studies significantly increased diagnostic accuracy for certain syndromes. Continuous research and adaptation in clinical practices remain essential for maximizing the benefits of EMG in neuromuscular assessments.
How to Use an EMG Machine for Muscle Testing and Analysis? - Clinical Implications of EMG: Diagnosing Neuromuscular Disorders
| Test Type | Purpose | Key Findings | Clinical Implications |
|---|---|---|---|
| Surface EMG | Assess muscle activation | Muscle activation patterns during movements | Guides rehabilitation protocols |
| Needle EMG | Identify nerve and muscle disorders | Denervation and reinnervation potentials | Aids in diagnosis of conditions like ALS |
| Maximal Voluntary Contraction | Evaluate muscle strength | Force output compared to normative data | Supports diagnosis of myopathies |
| Motor Unit Analysis | Assess motor unit health | Motor unit potentials and recruitment patterns | Indicates peripheral neuropathies |
Related Posts
-

How to Maximize Performance with Emg Machines in Rehabilitation Environments
-

Unlocking the Potential of the Best EMG Machine: Technical Specs & How to Optimize Performance for Global Buyers
-

Ultimate Guide to Choosing the Right Emg Machine for Your Business Needs
-

Top Strategies for Integrating Biofeedback Machines into Modern Wellness Programs
-

Top 10 EMG Equipment for Enhanced Muscle Monitoring and Analysis?
-
Ultimate Checklist for Choosing the Best Ecg Equipment for Your Clinic

